7 Point Plan
Diarrhoeal diseases:
The basics
 Diarrhoea is defined as having loose or watery stools at least three times per
day, or more frequently than normal for an individual. Though most episodes of
childhood diarrhoea are mild, acute cases can lead to significant fluid loss and
dehydration, which may result in death or other severe consequences if fluids
are not replaced at the first sign of diarrhoea.
Diarrhoea is defined as having loose or watery stools at least three times per
day, or more frequently than normal for an individual. Though most episodes of
childhood diarrhoea are mild, acute cases can lead to significant fluid loss and
dehydration, which may result in death or other severe consequences if fluids
are not replaced at the first sign of diarrhoea.
What causes diarrhoea?
Diarrhoea is a common symptom of gastrointestinal infections caused by a wide range of pathogens,
including bacteria, viruses and protozoa. However, just a handful of organisms are responsible for most
acute cases of childhood diarrhoea.
8 Rotavirus is the
leading cause of acute diarrhoea, and is responsible for about 40 per cent of all hospital admissions due
to diarrhoea among children under five worldwide.
9
Other major bacterial pathogens include
E. coli, Shigella, Campylobacter and
Salmonella, along
with
V. cholerae during epidemics (
Box 1).
Cryptosporidium
has been the most frequently isolated protozoan pathogen among children seen at
health facilities and is frequently found among HIV-positive patients (
Box 2). Though cholera is
often thought of as a major cause of child deaths due to diarrhoea, most cases occur among adults and older children.
How are diarrhoea pathogens transmitted?Most pathogens that cause diarrhoea share a
similar mode of transmission – from the stool of one person to the mouth of another. This is
known as faecal-oral transmission. There may be differences, however, in the number of organisms
needed to cause clinical illness, or in the route the pathogen takes while travelling between
individuals (for example, from the stool to food or water, which is then ingested).
What are the main forms of acute childhood diarrhoea?
There are three main forms of acute childhood diarrhoea, all of which are potentially life-threatening
and require different treatment courses:
- Acute watery diarrhoea includes cholera and is associated with significant fluid loss and rapid
dehydration in an infected individual. It usually lasts for several hours or days. The pathogens that
generally cause acute watery diarrhoea include V. cholerae or E. coli bacteria, as well as rotavirus.
- Bloody diarrhoea, often referred to as dysentery, is marked by visible blood in the stools. It is
associated with intestinal damage and nutrient losses in an infected individual. The most
common cause of bloody diarrhoea is Shigella, a bacterial agent that is also the most common cause of severe cases.
- Persistent diarrhoea is an episode of diarrhoea, with or without blood, that lasts at least 14 days.
Undernourished children and those with other illnesses, such as AIDS, are more likely to develop
persistent diarrhoea. Diarrhoea, in turn, tends to worsen their condition.
Why are children more vulnerable?
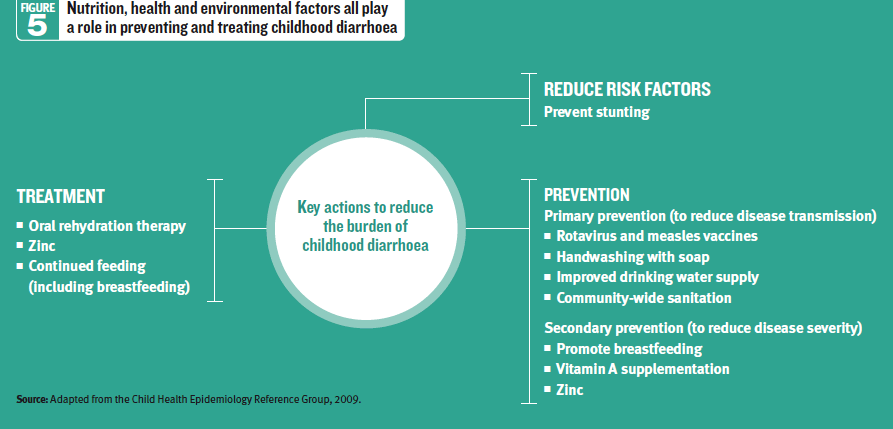
Children with poor nutritional status and overall health, as well as those exposed to poor environmental
conditions, are more susceptible to severe diarrhoea and dehydration than healthy children
(Figure 5). Children are also at greater risk than adults of life-threatening dehydration since water
constitutes a greater proportion of children’s bodyweight. Young children use more water over the
course of a day given their higher metabolic rates, and their kidneys are less able to conserve water compared to older children and adults.
How is diarrhoea prevented?
Reducing childhood diarrhoea requires interventions to make children healthier and less likely to
develop infections that lead to diarrhoea; clean environments that are less likely to transmit
disease; and the support of communities and caregivers in consistently reinforcing healthy behaviours and practices over time.

Many well-known child survival interventions are critical to reducing child deaths from diarrhoea.
They work in two ways: by either directly reducing a child’s exposure to the pathogens that cause
diarrhoea (through the provision of safe drinking water, for example) or by reducing a child’s
susceptibility to severe diarrhoea and dehydration (through improved nutrition and overall health).
WATER, SANITATION AND HYGIENE
Improvements in access to safe water and adequate sanitation, along with the promotion of
good hygiene practices (particularly handwashing with soap), can help prevent childhood diarrhoea.
In fact, an estimated 88 per cent of diarrhoeal deaths worldwide are attributable to unsafe water,
inadequate sanitation and poor hygiene.
14
Water, sanitation and hygiene programmes typically include a number of interventions that work to
reduce the number of diarrhoea cases. These include: disposing of human excreta in a sanitary
manner, washing hands with soap, increasing access to safe water, improving water quality at
the source, and treating household water and storing it safely.
Improvements in sanitation reduce the transmission of pathogens that cause diarrhoea by preventing
human faecal matter from contaminating environments. Improving sanitation facilities has been
associated with an estimated median reduction in diarrhoea incidence of 36 per cent across reviewed
studies.
15 (A recent survey in the
British Medical Journal showed that their readers believed sanitation to be the most important medical milestone
since 1840.
16) However, a major challenge in this
regard is scaling up sanitation facilities to the point where they are used by an entire community (‘total
sanitation’). Use of such facilities by
all community members is necessary to significantly reduce
diarrhoeal disease transmission (
Box 3).
17

Washing one’s hands with soap is another
important barrier to transmission (
Box 4), and has been cited as one of the most cost-effective public health
interventions.
19 A number of studies have
shown that handwashing with soap can reduce the incidence of diarrhoeal disease by over 40 per
cent.
20 Accessible and plentiful water has also been
shown to encourage better hygiene, handwashing in particular, although the extent to which access
to improved water sources reduces diarrhoea rates often depends on the type of water source available
(such as public taps or standpipes, protected dug wells or boreholes).
21
Interventions to improve water quality at the source, along with treatment of household water and
safe storage systems, have been shown to reduce
diarrhoea incidence by as much as 47 per cent.
22
Proven and field-tested household water treatment options that are currently being promoted include
chlorination, filtration, combined flocculation and disinfection, boiling, and solar disinfection. Household
water treatment could potentially be scaled up quickly and inexpensively in both development and
emergency situations. It has even become common practice in large cities where homes are connected
to a municipal water supply, since water is often polluted between the source and the point of use.
 ADEQUATE NUTRITION
ADEQUATE NUTRITION
Undernourished children are at higher risk of suffering more severe, prolonged and often more
frequent episodes of diarrhoea. Repeated bouts of diarrhoea also place children at a greater risk of
worsening nutritional status due to decreased food intake and reduced nutrient absorption, combined
with the child’s increased nutritional requirements during repeated episodes.
Diarrhoea often leads to stunting in children due to its association with poor nutrient absorption
and appetite loss. The risk of stunting in young children has been shown to increase significantly
with each episode of diarrhoea,23 and diarrhoea
control, particularly in the first six months of life, may help to reduce stunting prevalence
among children.24
 BREASTFEEDING
BREASTFEEDING
Breastmilk contains the nutrients, antioxidants, hormones and antibodies needed by
a child to survive and develop. Infants who are exclusively breastfed
for the first six months of life and continue to be breastfed until two
years of age and beyond develop fewer infections and have less severe
illnesses than those who are not, even among children whose mothers are
HIV-positive. This protection has been shown to be higher where maternal
literacy is lower and where sanitation is worse.
25
Infants who are not breastfed have a sixfold greater risk of dying from
infectious diseases in the first two months of life, including from
diarrhoea, than those who are breastfed.
26
MICRONUTRIENT SUPPLEMENTATION
Vitamin A supplementation is a critical preventive measure, and
studies have shown mortality reductions ranging from 19 per cent to 54
per cent in children receiving supplements.
27 This reduction is
associated in large part with declines in deaths due to diarrhoeal
diseases and measles. Vitamin A supplementation has also been shown to
reduce the duration, severity and complications associated with
diarrhoea.
28
Adequate zinc intake among children is critical for normal growth
and development. Recent supplementation trials have shown that adequate
zinc leads to a substantial reduction in childhood diarrhoea cases.
29
IMMUNIZATION
Immunizations help reduce deaths from diarrhoea in two ways: by helping
prevent infections that cause diarrhoea directly, such as rotavirus, and
by preventing infections that can lead to diarrhoea as a complication of
an illness, such as measles.
Rotavirus is estimated to cause about 40 per cent of all hospital
admissions due to diarrhoea among children under five years of age
worldwide
30 – leading to some 100 million episodes of acute diarrhoea
each year that result in 350,000 to 600,000 child deaths.
31 Introduction
of rotavirus vaccine in countries with the greatest diarrhoea burdens,
especially in Asia and Africa, must be accelerated on a priority basis.
Global rotavirus vaccine introduction has recently been recommended by
the World Health Organization (WHO).
32
Measles is an acute viral infection that is often self-limiting. But some children, particularly those who are
undernourished or have compromised immune systems, may experience serious side effects, including diarrhoea. Diarrhoea is one of the most
common causes of death associated with measles worldwide.

How is diarrhoea diagnosed?
Guidelines for the diagnosis and treatment of childhood diarrhoea are set out in the
Integrated
Management of Childhood Illness handbook.
33
Diagnosis is based on clinical symptoms, including the extent of dehydration, the type of diarrhoea
exhibited, whether blood is visible in the stool, and the duration of the diarrhoea episode. Treatment
regimens differ based on the outcomes of this clinical assessment. Microbiological culture and
microscopy are not necessary to diagnose diarrhoea and initiate treatment, even in high-income countries,
although these tools can help identify specific pathogens for outbreak investigations.
It is important that caregivers recognize the symptoms that require immediate attention from
appropriate health personnel, including trained community health workers. These symptoms
include dehydration, blood in the stool, profuse and persistent diarrhoea and repeated vomiting.
How is diarrhoea treated?
The latest recommendations for treating childhood diarrhoea in the developing world are set out in a
UNICEF and WHO joint statement
34 issued in 2004.
These interventions are proven, affordable and relatively straightforward to implement.
Since the 1970s, oral rehydration therapy has been the cornerstone of treatment programmes to prevent
life-threatening dehydration associated with diarrhoea (
Box 5). Fluid replacement should begin at
home and be administered by the caregiver at the start of the diarrhoea episode. A solution made from
oral rehydration salts (ORS) is the ‘gold standard’ of oral rehydration therapy, and a new formula has
been developed (known as low-osmolarity ORS) that improves overall outcomes when compared
to the original version (
Box 6). UNICEF and WHO recommend that all children with diarrhoea have
access to this new ORS formula; making it widely available to children in need will require innovative delivery strategies.
When ORS are not available, other fluids will also work to prevent dehydration among children with
diarrhoea, although they are not as effective in treating children who have become dehydrated.
Such fluids (which many countries have designated as ‘recommended homemade fluids’) can be prepared at home using readily available and
low-cost ingredients. Examples of rehydrating fluids include cereal-based drinks made from a
thin gruel of rice, maize, potato or other readily available low-cost grain or root crop the family has
at home. Breastmilk is also an excellent drink for fluid replacement and should continue to be given
to infants with diarrhoea simultaneously with other oral rehydration solutions.


If ORS or other appropriate fluids are not available, increased amounts of almost any fluid could also
help to prevent dehydration. Continuing to feed the child during the diarrhoea episode, while providing
oral rehydration therapy, further supports the absorption of fluids from the gut into the bloodstream
to prevent dehydration. Children receiving food during the diarrhoea episode are also more
likely to maintain their nutritional status and their ability to fight infection.
A recent and important development in diarrhoea treatment is the addition of zinc to the regimen.
Box 7 details the added value of zinc in diarrhoea treatment, and its effectiveness in reducing both the
duration and severity of diarrhoea episodes as well as reducing stool volume and the need for advanced
medical care. Children receiving zinc often have greater appetites and are more active during the
diarrhoea episode; its use has also been associated with increased ORS uptake. The provision of zinc
tablets by health workers may also reduce the demand from caregivers for other less effective drugs,
such as antibiotics and antidiarrhoeal medications, which should not be routinely administered.





 Diarrhoea is defined as having loose or watery stools at least three times per
day, or more frequently than normal for an individual. Though most episodes of
childhood diarrhoea are mild, acute cases can lead to significant fluid loss and
dehydration, which may result in death or other severe consequences if fluids
are not replaced at the first sign of diarrhoea.
Diarrhoea is defined as having loose or watery stools at least three times per
day, or more frequently than normal for an individual. Though most episodes of
childhood diarrhoea are mild, acute cases can lead to significant fluid loss and
dehydration, which may result in death or other severe consequences if fluids
are not replaced at the first sign of diarrhoea.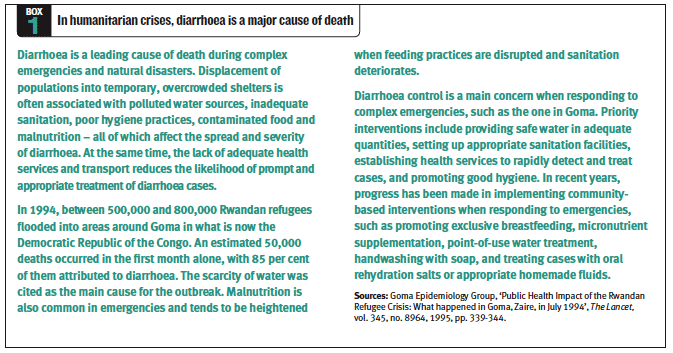

 Washing one’s hands with soap is another
important barrier to transmission (Box 4), and has been cited as one of the most cost-effective public health
interventions.19 A number of studies have
shown that handwashing with soap can reduce the incidence of diarrhoeal disease by over 40 per
cent.20 Accessible and plentiful water has also been
shown to encourage better hygiene, handwashing in particular, although the extent to which access
to improved water sources reduces diarrhoea rates often depends on the type of water source available
(such as public taps or standpipes, protected dug wells or boreholes).21
Washing one’s hands with soap is another
important barrier to transmission (Box 4), and has been cited as one of the most cost-effective public health
interventions.19 A number of studies have
shown that handwashing with soap can reduce the incidence of diarrhoeal disease by over 40 per
cent.20 Accessible and plentiful water has also been
shown to encourage better hygiene, handwashing in particular, although the extent to which access
to improved water sources reduces diarrhoea rates often depends on the type of water source available
(such as public taps or standpipes, protected dug wells or boreholes).21 ADEQUATE NUTRITION
ADEQUATE NUTRITION BREASTFEEDING
BREASTFEEDING
